Stage 3 Lyme Disease Signs
Stage 3 Lyme Disease is called late disseminated Lyme disease and the bacteria has spread throughout the body.
Stage 3 Lyme Disease Signs involves symptoms in various organs. Symptoms may include; arthritis of one or multiple large joints (usually the knee), confusion, short-term memory loss, inflammation of the heart, inflammation of tissue surrounding the brain, and numbness in the hands, legs and feet. For some patients, symptoms persist for months or years.
Stage 3 Lyme Disease Signs:
Within a few weeks (up to 2 years) after the start of the infection, about 60% of people develop arthritis characterized by joint pain and swelling. In stage 3, you may have temporary periods of arthritis or you may feel the arthritis symptoms all the time. You may also have ongoing nervous system problems, but this is less likely.
Symptoms of nervous system problems during stage 3 may include:
- Numbness or tingling in your hands and feet
- Trouble concentrating
- Slowed speech or language deficits
- Muscle weakness in your arms or legs
- Depression/anxiety/personality changes
Courtesy Of: http://www.cumc.columbia.edu
Lyme disease and how it can affect the brain and nervous system
Patients with neurologic symptoms should discuss with their doctor about having a lumbar puncture to remove and check spinal fluid for antibodies of the Lyme disease causing bacteria. When the spinal fluid (SF) is examined, it should be sent for testing of the bacterial PCR (Polymerase chain reaction), to look at the DNA of the bacteria, along with a blood sample to calculate a ratio index of bacteria and antibodies present within the patient. Please note, the blood should be drawn on the same day as the spinal fluid for an optimal study. The index refers to the ratio of bacterial antibodies in the SF compared to the antibodies present in the blood, to calculate the immune response levels in the whole body. When the index is positive, that indicates that there is a higher production of antibodies in the SF – a finding strongly suggestive of central nervous system invasion by the agent of Lyme disease. It is believed that the index may remain positive long after the initial infection has been treated due to immunologic memory. Unfortunately, patients may have neurologic Lyme disease, but test negative on the Lyme index, providing a false negative. When positive however, the clinician can be confident that this particular individual has or has had central nervous system Lyme disease.
MRI
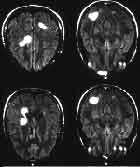
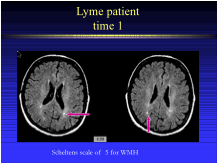
Unlike other images that assess brain function, a MRI captures the physical structure of the brain. Inflammatory abnormalities in the brain are also assessed with MRI scans. In children with neurologic Lyme disease, the MRI may reveal areas of increased white matter suggestive of inflammation or areas of decreased nerve function (see photo to the right). Up to 40% of adults with Lyme disease may have small white matter hyperactive areas as well. Certain factors, such as ischemic disease or a history of smoking, may result in increased number of white areas. In some patients, antibiotic treatment results in a decrease or disappearance of these white matter spots. The brain MRI of the young patient (to the right) revealed white lesions in this individual who had a fully positive IgG Lyme Western blot, indicating immune reactivity against the agent of Lyme disease.
***Because an MRI scan uses a very powerful magnet, patients with pacemakers or other metallic implants should not get an MRI.
Neuro-psychological Testing
Comprehensive cognitive assessments are valuable for several reasons. First, they provide an objective measurement of the person’s cognitive functioning at a specific point in time. Second, the testing is a useful way to monitor changes in response to treatment for patients with cognitive deficits. Third, neuro-psychological tests may help to differentiate the cause of cognitive problems; organic, neurologic, or psychiatric. Fourth, an understanding of deficits may help guide the use of alternate strategies to cope with the cognitive deficits; for example, a person with auditory attention problems may do best with visually presented information.
Since subjective reports of cognitive difficulties, such as memory problems, do not always correlate with objective data, we cannot rely only on self-reported cognitive problems. A comprehensive selection of tests is administered including; measures of intellectual functioning, verbal and visual memory, learning style, attention/concentration, verbal fluency, processing speed, and fine/gross motor functioning is administered. Impairments in working (short term) memory, attention, mental activation, language ability, and motor function have been documented in adults with Lyme disease. The most consistently identified deficits in adults with Lyme disease have been problems with verbal memory, verbal fluency and mental processing speed.
Studies by Keilp, Kaplan, Krupp and others support the hypothesis that cognitive impairments are caused by CNS dysfunction and not secondary to a psychological response to chronic illness. Subjective memory impairments may however be higher in LD patients with comorbid depression, a finding which strengthens our recommendation that patients with depression should be monitored closely by a psychopharmacologist.
